Varicose Veins & Venous Disorder
Introduction
Varicose veins and spider veins are common venous conditions that affect many adults. These conditions occur when the valves inside the veins do not function properly, causing blood to collect in the veins instead of flowing efficiently back to the heart. Over time, this increased pressure causes the veins to enlarge, become visible, and sometimes lead to discomfort or other complications. Varicose veins usually appear as enlarged, twisted veins on the legs and can cause symptoms such as pain, heaviness, swelling, or skin changes. Spider veins, on the other hand, are smaller, thin veins visible near the surface of the skin and are often considered a cosmetic concern, although they may sometimes cause mild discomfort. Early diagnosis and proper treatment can help manage symptoms, prevent complications, and improve quality of life. A vascular specialist can evaluate the condition and recommend the most suitable treatment based on the severity of the vein disorder.
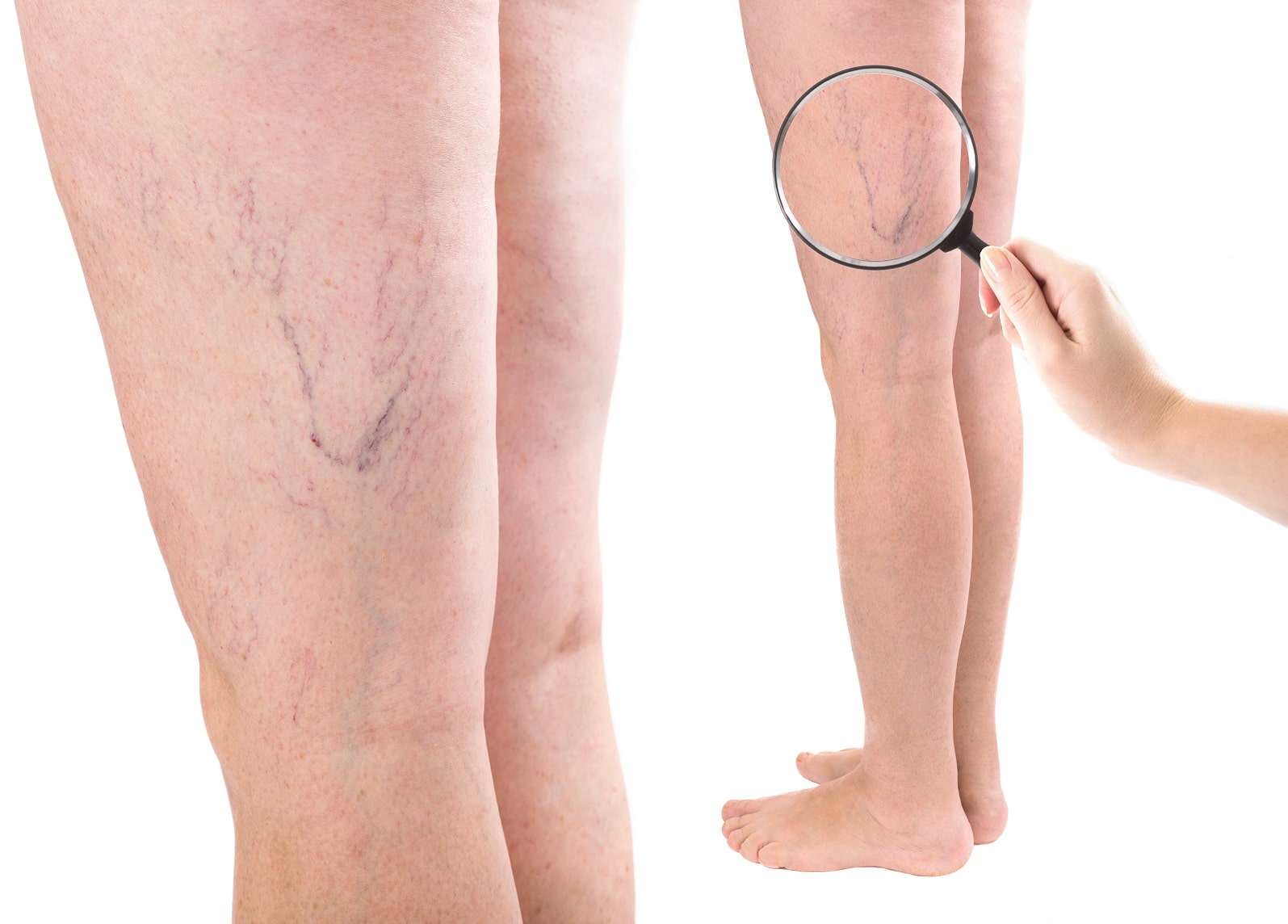
What Are Varicose Veins?
Varicose veins are enlarged veins that develop when the valves inside the veins become weak or damaged. Veins contain one-way valves that help blood move from the legs back toward the heart. When these valves stop functioning properly, blood can flow backward and collect inside the veins.
This increased pressure causes the veins to stretch and enlarge, resulting in the bulging and twisted veins that are visible on the skin surface. Varicose veins most commonly affect the legs because standing and walking increase pressure in the lower body veins.
The condition is often associated with chronic venous insufficiency, a long-term condition in which veins struggle to return blood efficiently to the heart.
Common Symptoms of Varicose Veins
Varicose veins may be visible before symptoms appear. However, many patients experience discomfort or other symptoms that affect daily activities.
Common symptoms include:
- Prominent blue or purple veins visible on the legs
- Leg heaviness or tiredness, especially after standing for long periods
- Aching or throbbing pain in the legs
- Swelling in the lower legs or ankles
- Burning or itching sensation around the veins
- Night cramps in the legs
- Skin discoloration around the affected veins
- Thickening or hardening of the skin in severe cases
In advanced stages, untreated varicose veins may lead to venous ulcers, which are wounds that usually appear near the ankles and can be difficult to heal.
Causes and Risk Factors
Several factors can increase the risk of developing varicose veins. These factors may affect the strength of vein walls or the function of vein valves.
Risk Factor | Explanation |
Age | As people age, veins may lose elasticity and valve function may weaken |
Family History | Genetics play a significant role in vein disorders |
Pregnancy | Increased blood volume and hormonal changes place extra pressure on veins |
Obesity | Excess body weight increases pressure on leg veins |
Prolonged Standing or Sitting | Limited movement affects blood circulation |
Hormonal Changes | Hormones may weaken vein walls in some individuals |
Previous Vein Problems | Past conditions such as blood clots may damage veins |
These factors can contribute to increased pressure in the veins, leading to vein enlargement and the development of varicose veins.
When Should You Consult a Vascular Specialist?
While some people seek treatment for cosmetic reasons, medical evaluation is important when symptoms begin to affect daily life.
Consult a vascular specialist if you experience:
- Persistent leg pain or heaviness
- Swelling in the legs or ankles
- Skin discoloration near the veins
- Bleeding from varicose veins
- Itching or burning sensation around the veins
- Non-healing wounds near the ankle region
Early diagnosis allows doctors to recommend treatments that can relieve symptoms and prevent complications
Diagnosis of Varicose Veins
A vascular specialist usually begins the evaluation with a physical examination and a review of symptoms. The doctor may also recommend imaging tests to assess blood flow in the veins.
The most common diagnostic test is:
Duplex Ultrasound
This non-invasive test uses sound waves to evaluate blood flow and identify damaged valves inside the veins. It helps determine the severity of the condition and assists in planning the appropriate treatment.
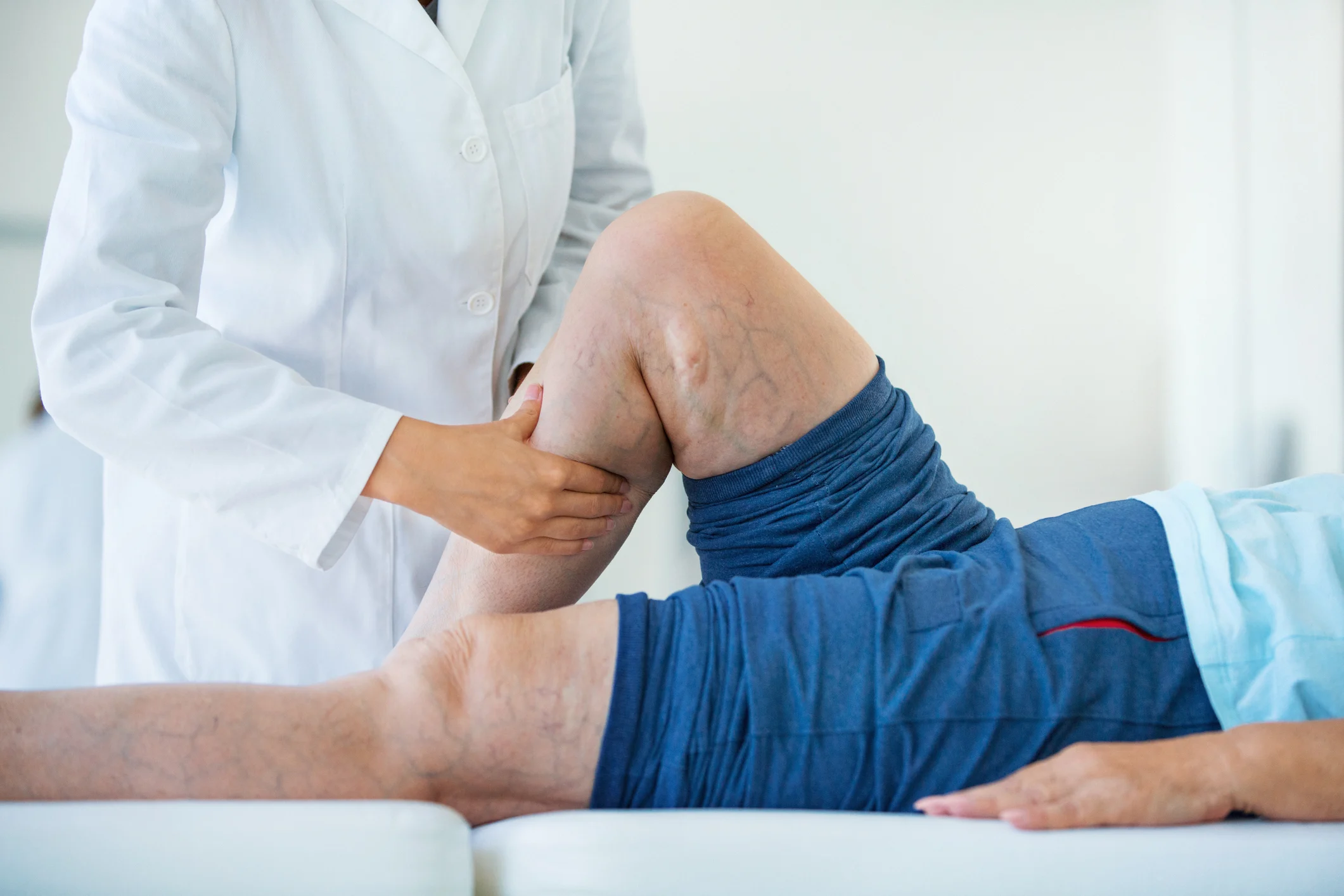
Treatment Options for Varicose Veins
Treatment for varicose veins depends on the severity of the condition, the symptoms experienced by the patient, and the underlying cause. Many modern treatments are minimally invasive and allow patients to resume normal activities quickly.
Lifestyle Changes and Home Care
For mild symptoms, certain lifestyle adjustments may help manage discomfort and improve circulation. Common recommendations include:
- Maintaining a healthy body weight
- Regular physical activity such as walking
- Avoiding long periods of sitting or standing
- Elevating the legs while resting
- Wearing compression stockings to support blood flow
These measures may help reduce symptoms but may not eliminate existing varicose veins.
Compression Therapy
Compression stockings apply gentle pressure to the legs, which helps veins and muscles move blood more effectively toward the heart. They are often recommended as an initial treatment or as supportive therapy after medical procedures. Compression therapy can help reduce swelling, discomfort, and fatigue in the legs.
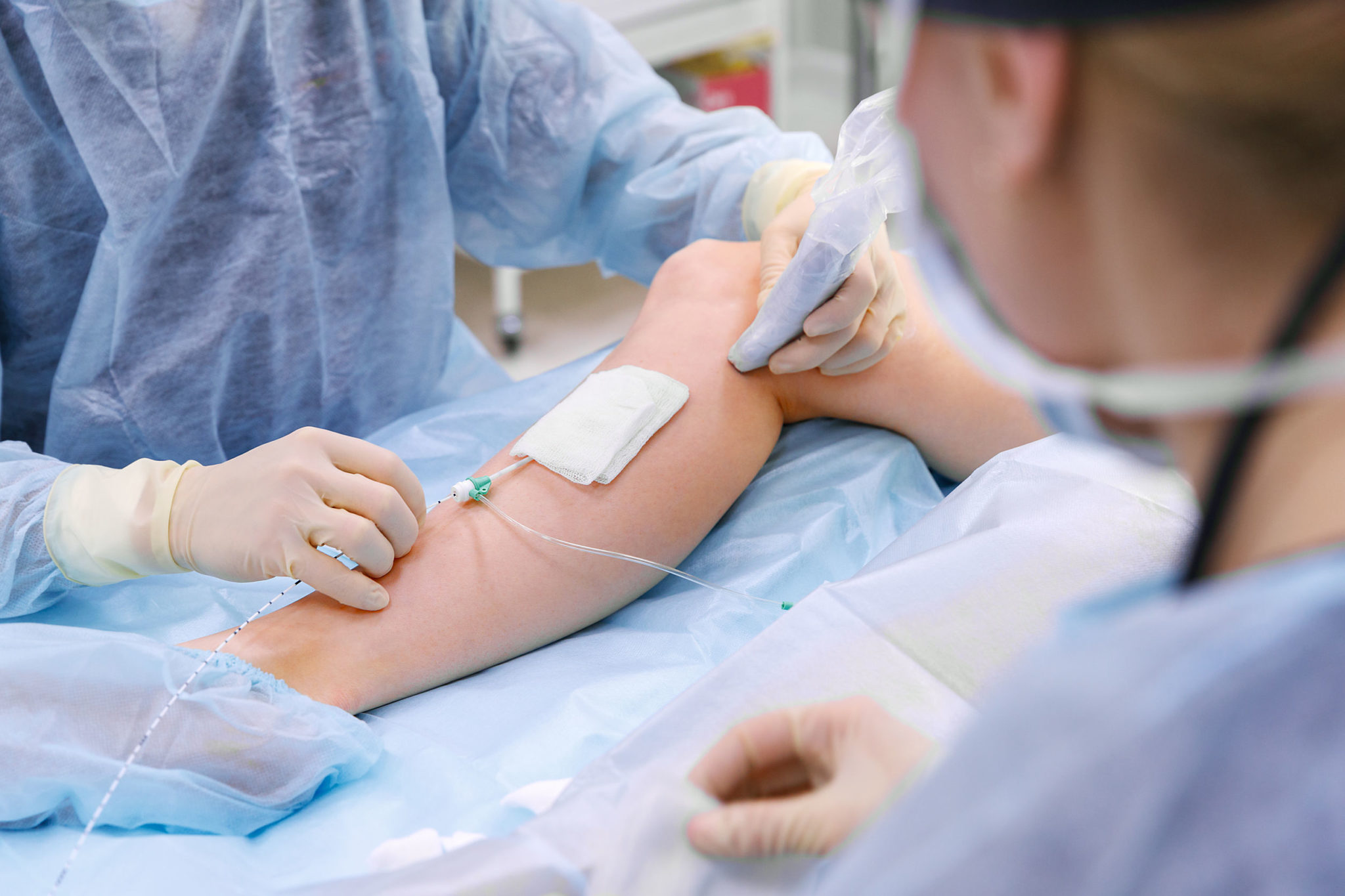
Minimally Invasive Treatments
Advancements in vascular medicine have made it possible to treat varicose veins using minimally invasive techniques. These treatments usually involve small incisions or injections and require minimal recovery time.
Sclerotherapy
Sclerotherapy involves injecting a special solution into the affected veins. This solution irritates the vein lining, causing the vein to collapse and eventually fade. The blood flow naturally redirects to healthier veins. Multiple sessions may be required depending on the number and size of veins being treated.
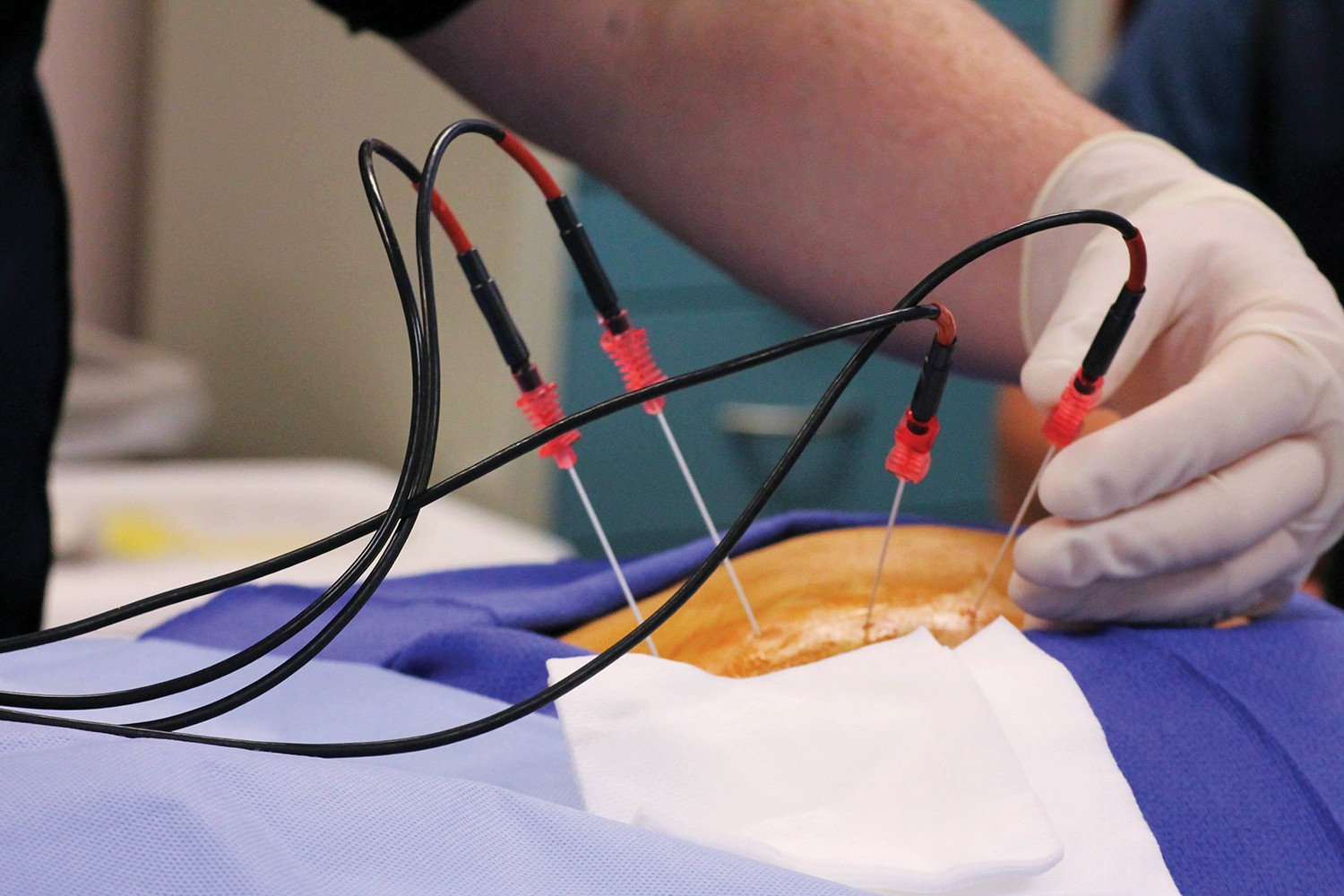
Ablation Therapy
Endovenous Laser Ablation (EVLA)
Endovenous Laser Ablation uses laser energy delivered through a small catheter inserted into the vein. The laser heat closes the affected vein, allowing blood to flow through healthier veins instead. This procedure is performed under local anesthesia and usually takes less than an hour.
Benefits include:
- Minimally invasive procedure
- Minimal discomfort
- Faster recovery time
- Effective for moderate to large varicose veins
Radiofrequency Ablation (RFA)
Radiofrequency ablation works similarly to laser treatment but uses radiofrequency energy to heat and close the affected vein. The procedure is guided by ultrasound and is commonly used for larger veins.
Advantages include:
- Quick procedure time
- Minimal scarring
- Reduced recovery period
- High success rate
Glue Ablation (VenaSeal)
Glue ablation is a newer treatment that uses a medical adhesive to close the affected vein. The adhesive seals the vein, allowing blood to reroute through healthy veins. Benefits of this technique include:
• No heat-based energy
• Minimal discomfort
• Quick recovery
• No need for compression stockings in some cases
Surgical Treatments
In certain advanced cases, surgical procedures may be recommended.
Vein Stripping and Ligation
This traditional surgery involves tying off and removing the affected veins. It is usually recommended when veins are very large or when other treatments are not suitable.
Ambulatory Phlebectomy
This procedure removes smaller varicose veins through tiny incisions in the skin. It is performed under local anesthesia and generally leaves minimal scarring.
Treatment Comparison
Treatment | Procedure Type | Recovery Time |
Compression Therapy | Non-invasive | Immediate |
Sclerotherapy | Injection procedure | 1–2 days |
Laser Ablation | Minimally invasive | 1–2 days |
Radiofrequency Ablation | Minimally invasive | 2–3 days |
Glue Ablation | Minimally invasive | 1–2 days |
Surgery | Invasive | About 1 week |
The most appropriate treatment depends on the size of the veins, severity of symptoms, and individual patient factors.
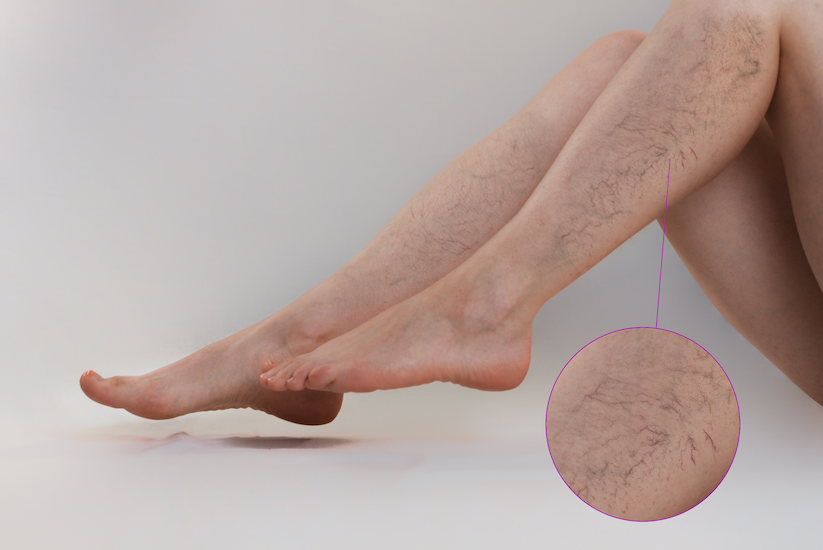
Spider Veins
What Are Spider Veins?
Spider veins are small, thin blood vessels visible just beneath the skin surface. They often appear as red, blue, or purple lines that resemble a spider web or branching tree pattern. Spider veins commonly develop on the legs or face. Although they are generally harmless, some individuals may experience mild symptoms such as aching, burning, or swelling in the affected area.
Why Do Spider Veins Appear?
Spider veins develop when tiny valves inside small veins stop functioning properly. This causes blood to pool in the vein, making it expand and become visible through the skin. Factors that may increase the risk of spider veins include:
- Age-related changes in veins
- Hormonal changes during pregnancy
- Family history of vein disorders
- Prolonged standing or sitting
- Excess body weight
- Sun exposure affecting facial veins
Spider veins are very common and affect a significant percentage of adults.

Treatment Options for Spider Veins
Treatment for spider veins is often sought for cosmetic reasons, although it may also help relieve mild symptoms.
Compression Stockings
Compression stockings improve circulation in the legs and may reduce discomfort associated with spider veins.
Sclerotherapy
Sclerotherapy is one of the most effective treatments for spider veins. A special solution is injected into the veins, causing them to collapse and gradually fade.
Laser Treatment
Laser therapy can target small spider veins using focused light energy. This technique is commonly used for veins that are too small for injections. Laser treatment usually requires multiple sessions for optimal results.
Why Choose Dr. Sravan for Varicose Veins Treatment in Bangalore
Dr. Sravan C.P.S, is a vascular and endovascular surgeon experienced in diagnosing and treating venous disorders such as varicose veins and spider veins. His treatment approach focuses on identifying the underlying vein problem and providing advanced, minimally invasive solutions that help patients achieve lasting relief. Dr. Sravan has been recognized among the Best Doctors in South India by Outlook Magazine, reflecting his commitment to excellence in vascular care and patient outcomes.
What Sets Dr. Sravan Apart
✔ Expertise in treating varicose veins, spider veins, and venous insufficiency
✔ Use of advanced minimally invasive procedures such as laser treatment and sclerotherapy
✔ Personalized treatment plans based on vein mapping and diagnostic imaging
✔ Focus on cosmetic improvement and long-term vein health
✔ Recognized among Best Doctors in South India – Outlook Magazine
Patients receive comprehensive care from diagnosis and treatment to follow-up management to prevent recurrence of varicose veins.
Preventing Varicose and Spider Veins
Although vein disorders cannot always be prevented, certain lifestyle measures may reduce the risk of developing them or help slow their progression. Helpful preventive steps include:
- Regular physical activity to improve circulation
- Maintaining a healthy body weight
- Avoiding long periods of standing or sitting
- Elevating the legs when resting
- Wearing supportive footwear
- Using compression stockings when recommended by a doctor
These measures can help support vein health and reduce pressure on the veins.

